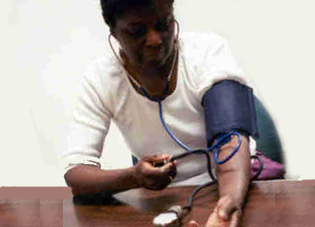
Monitoring your blood pressure
A Healthy Hearts Guide  ® ®
|
-
High blood pressure (HBP) affects two thirds of African- Americans with such devastating long-term affects as kidney damage, heart damage and stroke. African Americans who have a stroke suffer more extensive physical impairments that last longer than those of other racial groups.
The death rate for stroke is 79.8 percent higher in African-American women than white women. African Americans have a death rate from HBP that is about 4 1/2 times higher than the rate for white women.* We must work together with our healthcare professionals to control this silent killer
|
Who should monitor your blood pressure?
If you are on a program for control of high blood pressure, it is probably a good idea to
learn how to take your own blood pressure. By working in partnership with your
doctor, you can keep your blood pressure under better control.
Blood pressure kits can be purchased at
your local surgical supply store. The electronic digital type is easiest to use but
you may want to learn to use the standard blood pressure cuff with separate
stethoscope. While you may need someone to assist you with this type of blood pressure
device, the results are generally regarded as being more accurate. Whichever device
you choose, have it checked periodically against the most accurate mercury-type
device used by hospitals and doctors, and make sure you keep your
equipment in good working order.
When to take your blood pressure
You can take your blood pressure at any time
of the day but don’t take a reading just after smoking a cigarette or drinking a
beverage with caffeine or if you have a full bladder. Take your blood pressure when you
are relaxed and sitting up for at least 5 minutes.
How to take your blood pressure
Start by taking the blood pressure in
both arms. It is common for blood pressure readings to differ by as much as 10 points. If
the readings stay consistently similar, your doctor may suggest you use the arm with the
higher reading. Ask your doctor what range your blood pressure should be and what to do
should your blood pressure become too high or too low. Here are some other
guidelines:
- Sit at a table with your arm comfortably extended. When using a digital machine, note
the product instruction sheet for the best placement of your arm to increase the accuracy
of the reading.
- Place the cuff onto a bare upper arm. The cuff should fit snugly. It should wrap
easily around the upper arm with some overlap. The edge of the cuff should be about one
inch above the bend of the arm with the middle of the bladder (the rubber insert) over the
brachial artery (locate the brachial artery by gently depressing your index and middle
finger over the area and feeling for a pulse). Special cuffs are designed for those with a
large upper arm. An improper reading will result if using a regular cuff on an obese
person’s
- Inflate the cuff to 180 or as directed on the instructions. The numbers on the
digital scale will read on a screen when inflation and deflation have been
completed.
This is the number you record. Write down the date, time and blood pressure reading with
the higher number on the top and the lower number on the bottom (see example
of a completed Blood Pressure Record below)
Date |
Time |
BP |
Comments |
3/2/2000 |
10:00 am |
160/90 |
Forgot pills. Took 2 hours late.
|
3/3/2000 |
10:15 am |
132/72 |
Feeling better. Started DASH diet today.
|
If using a standard stethoscope and sphygmomanometer (blood pressure
apparatus), you may need some help in fastening the cuff and with holding the
bell of the stethoscope snug against your arm . Place the ear
pieces into you ears and the diaphragm over the middle bend of the arm where you felt the
brachial pulse — just below the edge of the cuff. Squeeze the bulb to inflate the
cuff quickly to 180 (or to 20 points above the last reading), then slowly and carefully
open the valve (located on the side of the bulb) to release the air. Listen carefully.
Note the number reading when you first heard sound and the number reading when
you last heard sound. Record both of these numbers.
Tools to help you monitor your blood pressure
Click here for a Blood Pressure Record to print out.
Click here for a step-by-step picture guide on how
to take your own blood pressure.
Note: blood pressure is measured in millimeters of mercury or “mm Hg.”.
The higher number is called the systolic pressure and is the pressure exerted on
artery walls when the heart is in the contracting phase. The lower number is the diastolic
pressure and is the pressure exerted on artery walls when the heart is in the resting
phase. In striving to achieve better management of high blood
pressure, new limits for normal were recently introduced by the World
Health Organization (WHO), recommending the systolic reading be less than 135 mm of Hg. and the
diastolic less than 85. When the bottom number goes above 85 and stays there,
then you are considered to have high blood pressure. Clinicians sometimes institute these values
when managing the care of diabetes or other conditions that place an individual at higher risk
for complications. For more information on high blood pressure go to www.nhlbi.nih.gov
* Stroke facts are from National Stroke Association.
|
Facts
|
Shortcut to Healthy Hearts
|
Annual Physical
|
Blood Pressure
|
Blood Pressure Log
|
Blood Pressure Monitoring
|
Taking Medicines Safely
|
Medicines Record
|
Menopause
|
Caregiver Support
|
Care Plan
|
Child Development Checklist
|
Safety Checklist for
Infants and Toddlers
|
Improve Doctor–Patient Communication
|
Path for a Healthy Heart
|
Taking Coumadin
|
Get Smart About Smoking
|
How to Quit Smoking
|
Heart Wellness
Back to top
Disclaimer | Donate Now | Contact Us | Site Map | Store
|
©1999-2000; updates: 2002, 2004, 2005, 2007 Women's Heart Foundation, Inc. All rights reserved.
Unauthorized use prohibited. The information contained in this Women's
Heart Foundation (WHF) Web site is not a substitute for medical advice or
treatment, and WHF recommends consultation with your doctor or health care
professional.
|
|
|

























